Conditions Commonly Linked To Back Pain
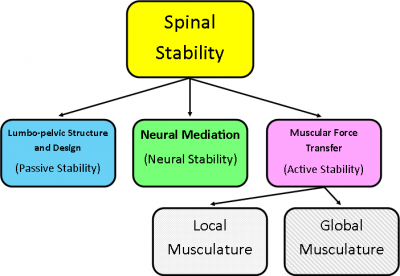
If you can remember I introduced the Panjabi (1992) concept of the three interlinking subsystems:
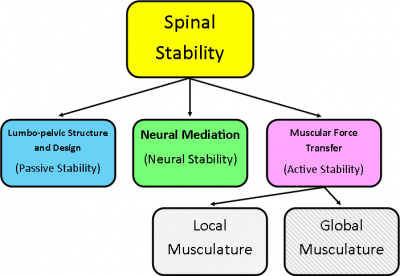
We discussed the discs which form part of the suspension system we have within our passive subsystem. Another part to that subsystem also has a significant role to play in spinal pathology – the spinal column (including all the bones and joints).
If the spinal column is stacked correctly with the right control from the core muscles things should be good, however age related change, trauma or prolonged postures can change this.
Osteoarthritis (OA) of the spine is common, often referred to as ‘spondylosis’. In the UK over 8 million people suffer with OA according to nhs.uk. Arthritis is a general term that describes many different diseases causing tenderness, pain, swelling, and stiffness of joints as well as abnormalities of various soft tissues of the body. The term comes from “arthros,” meaning a joint and its attachments, and “-itis,” meaning inflammation.
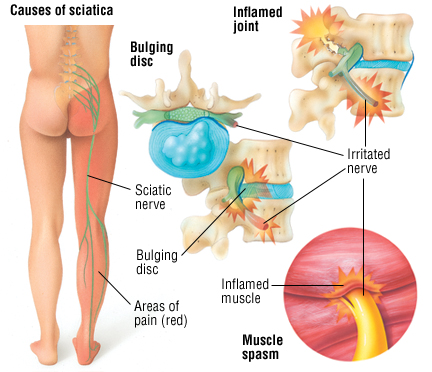
The below diagram highlights the changes to the articular surfaces caused by the OA. The key changes to note are the bone lipping / spurs that are created by the body building more bone to spread the load, increasing the surface area, and the narrowed disc space caused by potential disc damage or age related change. With the narrowed disc space, the back of the spine where the little facet joints are, are then pushed closer together increasing the wear and tear on those joints and again creating osteoarthritic changes when the cartilage is worn down and the joint surfaces inflame.
As you can see below the OA changes leading to inflammation around the facet joint, can also compress the exiting nerve root, which can lead to nerve pain. For example nerve pain coming from the lumbar spine (the low back area) is called sciatica.
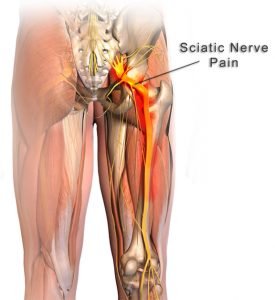
The nervous system is one continuous system; it is tethered at certain points so it doesn’t all drop to your feet when you stand up. Your nerves make up the control subsystem of the Panjabi theory. Nerves are made up like cables, with the threads of the cable being axons which communicate information to and from the brain and spinal cord. Compression of a nerve occurs when pressure is placed on a nerve, usually from swelling due to an injury, arthritic changes or pregnancy, and can result in pain, weakness, numbness or paralysis. Symptoms may be felt in areas far from the actual site of damage, a phenomenon called referred pain or a radiculopathy.
Nerve pain can often be worse at night when trying to sleep, but to date there is limited or no research about bed types, nerve pain and sleep quality. Potential causes for the increased symptoms could be due to a number of reasons, ranging from time to feel and think to prolonged sleeping positions causing aches and pains. But one of the most common reasons is due to your blood pressure dropping whilst you are relaxed and warm in bed. With the reduction in your blood pressure as you rest the push behind the oxygen cells to get them through the blood vessel walls to the nerve tissue reduces and the overall oxygen delivery reduces causing the nerve to become mildly hypoxic (lack of oxygen), which will make the nerve irritated and grumpy. If this occurs one of the best things to help is to move around and increase your blood pressure again.
So if you are suffering with joint or nerve pain, consider the following tips to help you choose a bed that will help you manage your pain but also get a good nights sleep. You should be considering the quality of the support the bed offers, your weight and the mattress type and the positions you tend to sleep in (mentioned in article 2).
- Stomach sleepers tend to like a medium firm mattress (as too firm = increased pressure on the knees and chest, and too soft = can allow excessive extension at the spinal joints pushing the facet joints together and potentially causing discomfort, and malalignment at the neck and head.)
- Side sleepers tend to prefer a medium to soft firmness of the mattress, as the pressure is more focused on the shoulders and hips which have a smaller surface area. So tend to also enjoy a medium to firm mattress with a memory foam topper, or popping a couple of pillows between the legs to reduce the twist at the back.
- Back sleepers tend to prefer medium to firm mattress as they have a larger surface area in contact with the bed, so like the support. However a back sleeper with a facet joint dysfunction / OA will potentially struggle as the firmness would promote extension through the spine which could increase their pain, so again a memory foam alternative may work to cushion the spine or pillows under the knees to take the load off the low back area.
The final subsystem that can exacerbate or improve symptoms is the active subsystem, the muscles and tendons etc. If certain muscles are tight, or muscles are imbalanced this can cause pain in the muscle, but also can pull on the bones that the muscles are attached too, causing a misalignment/pinching. So regular exercise and stretching is important to maintain the optimal length, strength and balance; consider pilates, yoga, tai chi style activities.
So in summary all 3 subsystems can contribute to spinal pain, a study in 2006 found that sleep quality is significantly affected by low back pain, and they also found that people’s sleep quality improved with a medium to firm mattress. Another study in 2008 in Applied Ergonomics highlighted that the age and quality of the bed had a major effect on their back pain, the newer and more moderately to expensively priced generally the better. So you do get what you pay for and you should also consider changing your mattress every 8-10 years.
Next time we will be discussing more peripheral joint problems (like shoulders and hips) and the best sleeping systems, including top tips for buying a new bed.
Until next time... sleep well.
Download Your Free Brochure
Sleeping on an old mattress or one that is not right for your body size, can also contribute to back stiffness, aches and pains.
To find out more about our collection of luxury mattresses and quality wooden beds, simply click on the link below to download your free brochure.
References
https://www.arthritis.org/diseases/osteoarthritis
http://www.nhs.uk/Conditions/Arthritis/Pages/Introduction.aspx
http://www.webmd.com/osteoarthritis/osteoarthritis-of-the-spine
http://www.mendmeshop.com/back/pulled-muscle-in-back.php
Grouped comparisons of sleep quality for new and personal bedding systems. Appl Ergon. 2008 Mar;39(2):247-54. Epub 2007 Jun 26.
Subjective rating of perceived back pain, stiffness and sleep quality following introduction of medium-firm bedding systems. J Chiropr Med. 2006 Winter;5(4):128-34.